DIALYSIS TYPES
Many people with Alport syndrome will face decisions about life-sustaining treatment. The more we know about those treatment options, the better we’ll be able to determine the best choice for ourselves and our family. While awaiting a life-saving transplant, many patients experience regular dialysis treatments.
A normal kidney does an amazing job of filtering waste products our of blood, eliminating extra fluid, balancing chemicals like sodium and producing certain hormones that help produce red blood cells and support bone health. As our kidney function declines, we need to find another way to provide our bodies with these same functions. Dialysis can help. There are two types of dialysis: hemodialysis and peritoneal dialysis.
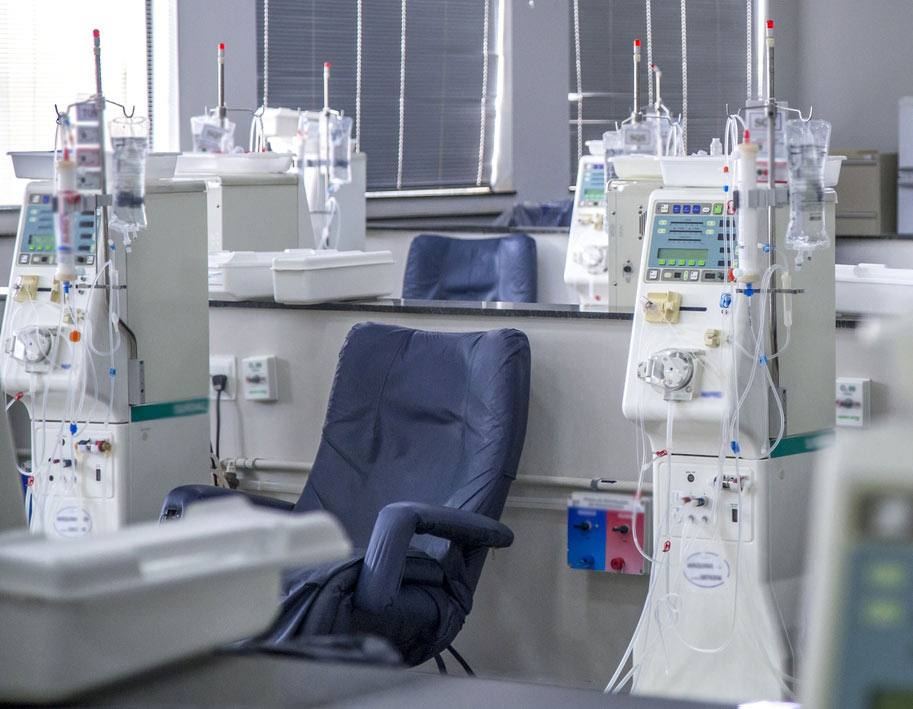
Hemodialysis
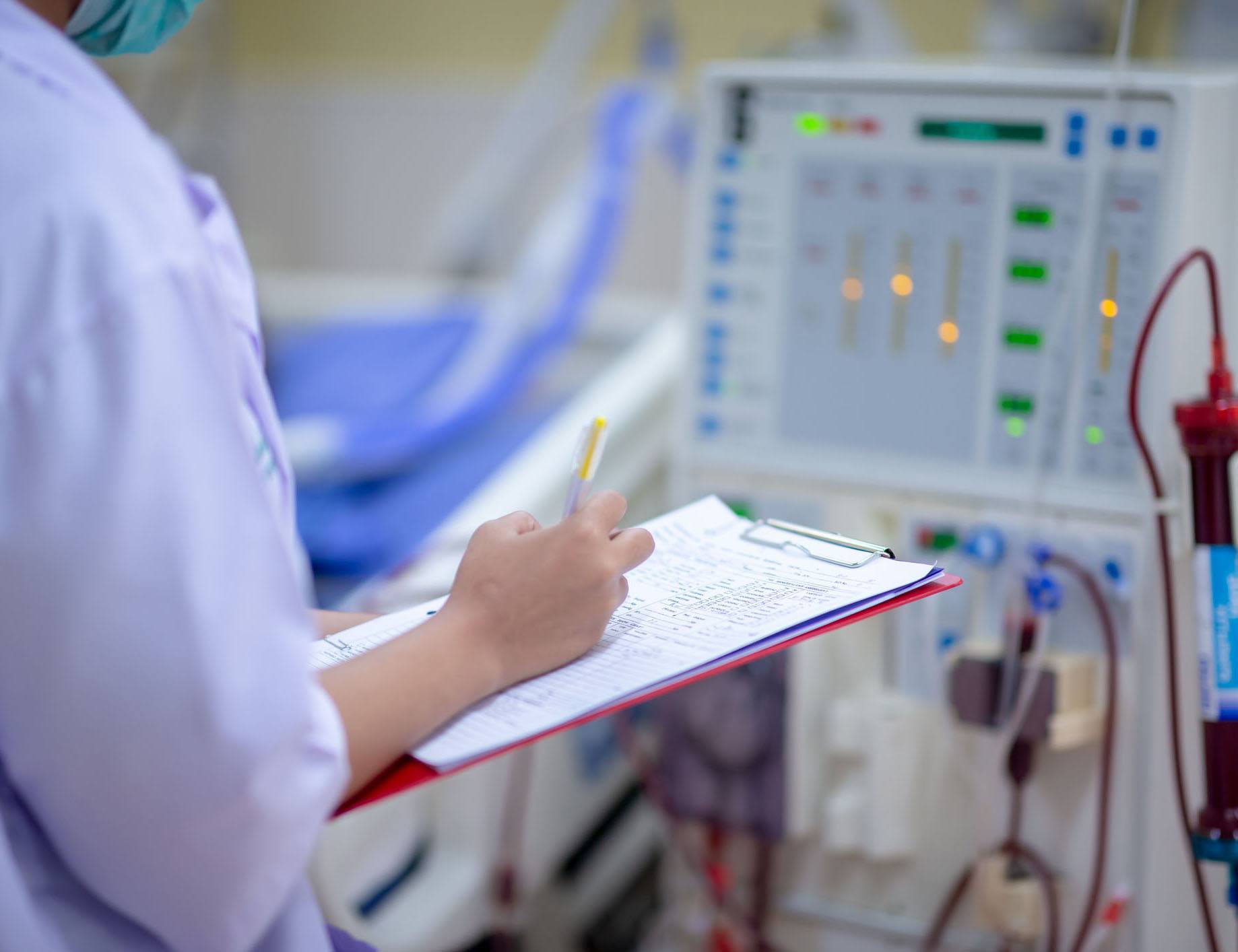
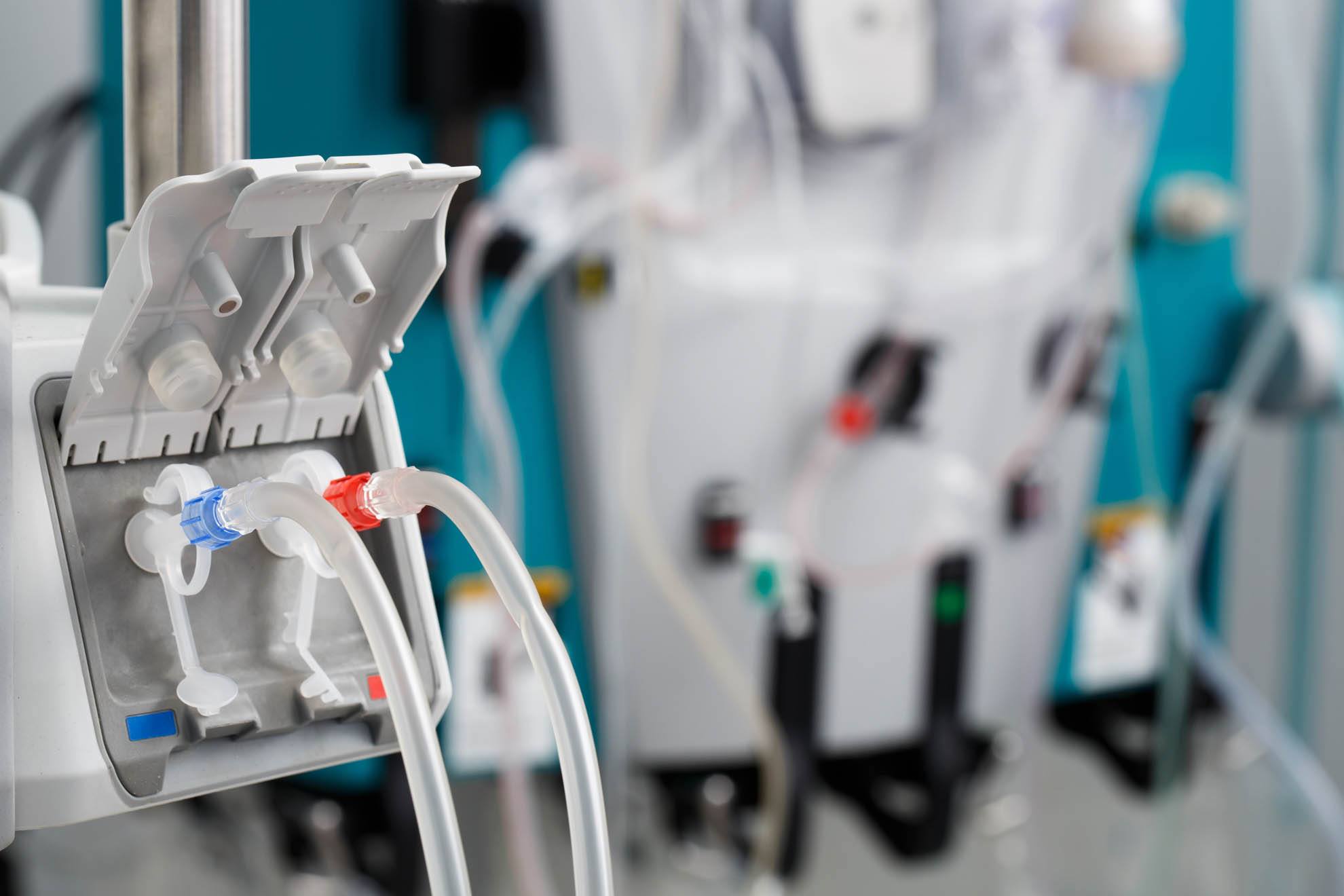
In hemodialysis, our blood passes through the fibers in an artificial kidney or dialyzer. These tiny hollow fibers allow waste and certain chemicals to migrate out of our blood, through the membrane of the fibers and into the solution that bathes the fibers within the plastic housing of the dialyzer. In addition, extra fluid can also be drawn off. Most people receiving hemodialysis treatments are scheduled in a clinic setting three days each week for about four hours each treatment.
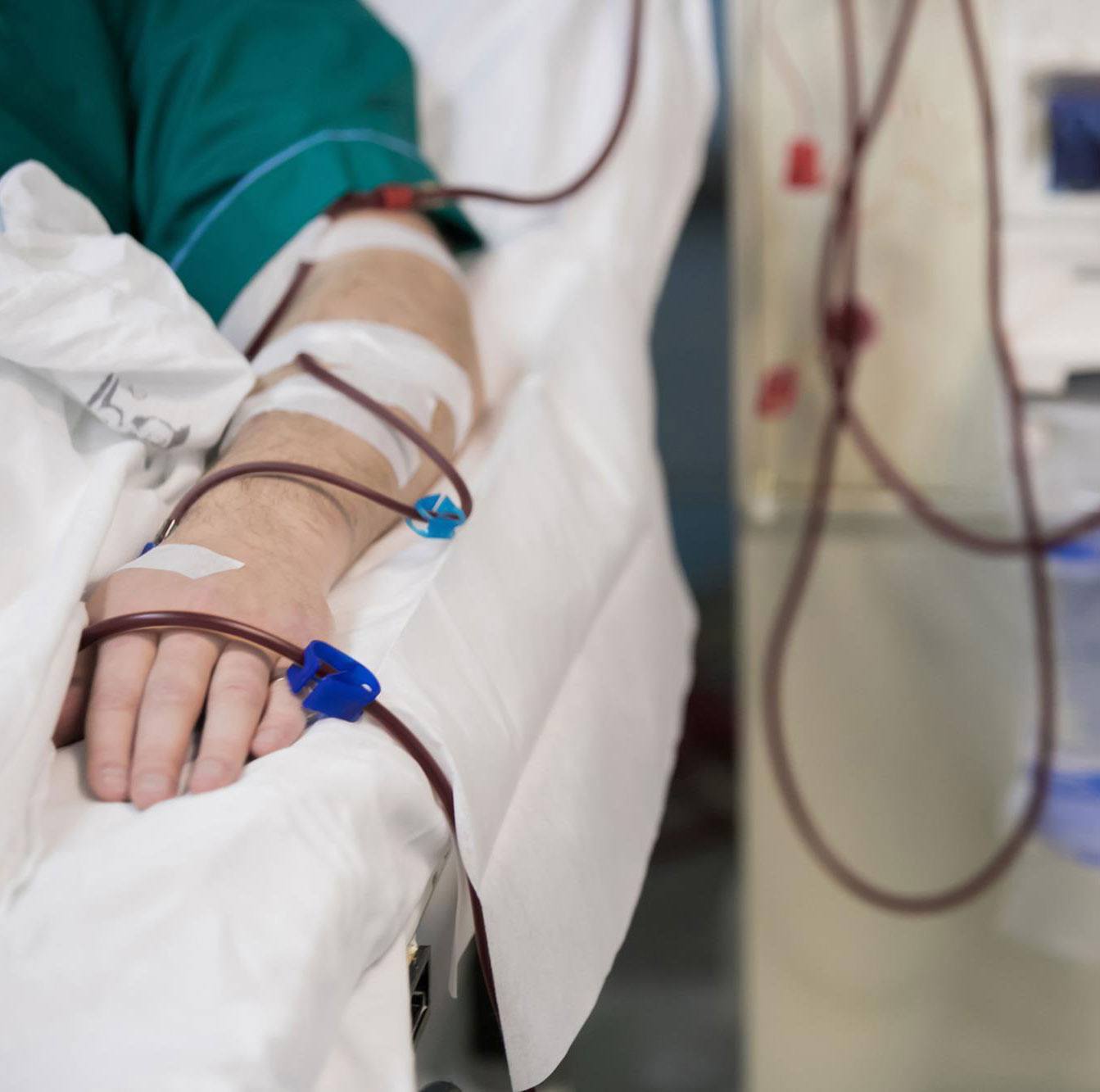
Registered Nurses and Dialysis Technicians are trained to initiate the treatment by placing two needles in a fistula (which is a surgically created modification of blood vessels), typically in your arm.
The blood is drawn off with one needle, and the cleaned blood is returned by the second. Some people receiving hemodialysis are trained with a partner, such as spouse or adult child, to perform the treatment at home.
In addition, there is a hybrid method of hemodialysis that is prescribed as daily short treatments also performed by the patient with a partner at home.
Peritoneal Dialysis
Peritoneal Dialysis also cleans the blood and moves extra fluid out of the body but instead of needles in a fistula, it uses the blood vessels in the abdominal lining (peritoneum).
A small tube is surgically placed through the abdominal wall through which a special solution is instilled at intervals, left in place for a period of hours then drained back out through the same little tube into a sterile collection bag and discarded.

During the time the fluid is in your abdominal cavity, the blood vessels in the abdominal lining function as the filter drawing waste and extra fluid out of the blood in those vessels.
Peritoneal dialysis is performed independently at home throughout the day or using a cycling device that allows the intervals to be managed while you sleep. There are fewer medications and fewer dietary restrictions for most patients using peritoneal dialysis.
In this video, Alport patient Chris Pak shares his former experience of daily CAPD (Continuous Ambulatory Peritoneal Dialysis) prior to receiving a renal transplant. As you’ll see, Chris performs “manual” exchanges – fills, dwells, and removal of dialysis fluid – without the use of a cycler machine. Parents/caregivers of pediatric patients can learn more about Peritoneal Dialysis at this link.
There are many factors that can influence your decision about what treatment option is best for you. Your nephrology team can provide more detailed information about each option.
For an excellent overview of dialysis options and the transplant process, watch our Ask the Experts Webinar hosted by Dr. James Simon (Cleveland Clinic).
Additionally, this National Institute of Health downloadable document contains more information so you can be your own best advocate as you consider how to receive dialysis.
In June 2023, CJASN published a patient perspective article “When Should Dialysis Be Started in Children and Young Adults with Kidney Failure?” written by ASF Executive Director Lisa Bonebrake
Further information on dialysis can be viewed at the following websites:
American Association of Kidney Patients
ESRD National Coordinating Center
Medicare’s website can help you better understand coverage due to End-Stage Renal Disease/dialysis treatment.
The Patient-Centered Outcomes Research Institute released study results in July 2021 about treating depression while on dialysis.
Information on this page provided by Alport syndrome patient & retired renal nurse, Janine Reed, RN, CDN.
