This is the second of three articles that will provide an overview of what we know about the three most studied genetic types of Alport syndrome, advances in genetic testing and how these advances may affect the understanding of Alport syndrome.
As discussed in the previous article in this series, Alport syndrome is caused by mutations in the type IV collagen genes. Type IV collagen is a family of six proteins, or chains, that are known as alpha-1 through alpha-6. Mutations that affect the alpha-3, alpha-4, and alpha-5 chains cause Alport syndrome. The alpha-3, 4, 5 chain is a major component of the basement membranes in the kidney, ears, and eyes.
Autosomal Recessive
The second most common form of Alport syndrome accounts for 15% of the cases and results from mutations of the alpha-3 or alpha-4 chain of type IV collagen (gene COL4A3 or COL4A4) and is called Autosomal Recessive Alport syndrome or ARAS.
Autosomal recessive disorders result when both copies of a gene are defective. Typically, each parent of a child with a recessive condition passes a mutant gene to the affected child. The genes COL4A3 and COL4A4 are located on chromosome 2. Each person has two copies of this chromosome, and two copies of both the COL4A3 and COL4A4 genes. The parents only have one mutation in one of the chromosomes and so they can have no symptoms or have some hematuria (blood in the urine). However, they will not have progression of the disease.
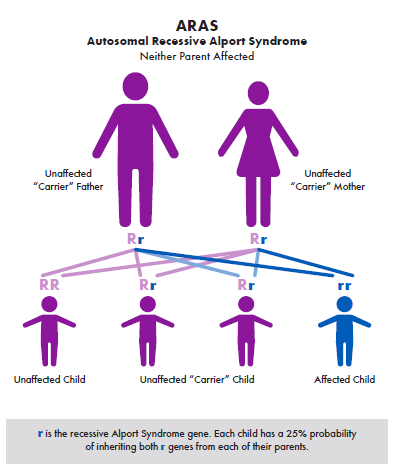
When each parent carries a mutation in COL4A3 or COL4A4, there is a 25% chance with every pregnancy that the child will have ARAS. Unlike X-linked Alport syndrome, the autosomal recessive type affects females just as severely as males. This is illustrated in the diagram above.
Autosomal Dominant
The least common form of Alport syndrome accounts for about 5% of the cases and results from mutations of the alpha-3 or alpha-4 chain of type IV collagen (gene COL4A3 or COL4A4) and is called Autosomal Dominant Alport syndrome or ADAS.
These patients have one mutant copy of the COL4A3 or COL4A4 gene. Mutation in one copy of COL4A3 or COL4A4 can cause progressive kidney disease and hearing loss. People with ADAS resemble people with XLAS, with some differences: kidney failure occurs relatively late in life (after age 40), changes in the eyes are very unusual and there is no difference in severity of disease in males and females. People with ADAS usually have a family history that is positive for progressive kidney disease and hearing loss. Mutation in one copy of COL4A3 or COL4A4 can also cause thin basement membrane nephropathy (TBMN), which differs from ADAS in that progressive kidney disease and hearing loss are very unusual. People with TBMN usually have a family history that is negative for progressive kidney disease and hearing loss. Researchers are still trying to understand why some people with these mutations have ADAS and others have TBMN.
Each child of an affected parent has a 50% chance of inheriting the mutation and this is illustrated in the diagram above.
Additional Resources:
Genetics on ASF website
Alport syndrome and Thin Basement Membrane Nephropathy by Dr. Clifford Kashtan
Other articles in our Alport syndrome Genetics series:
Part 1 of 3 – Alport syndrome Genetics 101: X-Linked
Part 3 of 3 – Alport syndrome Genetics 201: Understanding Specific Gene Mutations